Cervical cancer (cancer of the cervix) is the second most common cancer experienced by women world-wide. In Australia every year, around 800 women are diagnosed with cervical cancer. Half of these women have never had a Pap test.
The cervix is found at the lower part of the uterus, at the top of the vagina.
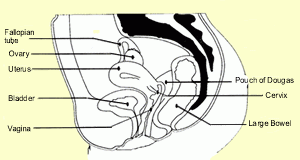 Squamous cell carcinoma is the most common form of cervical cancer and can be prevented (80-85 per cent) by regular Pap tests to detect early changes. The other form of cervical cancer is adenocarcinoma accounting for 12-15 per cent.
Squamous cell carcinoma is the most common form of cervical cancer and can be prevented (80-85 per cent) by regular Pap tests to detect early changes. The other form of cervical cancer is adenocarcinoma accounting for 12-15 per cent.
Cancer of the cervix is very rare under the age of 25 years, mostly occurring in the 55-60 year age group. The progression from high grade changes to cancer takes between 1 and 30 years with an average of 10 years.
Risk Factors
The risk factors for cancer of cervix are:
- Ever having sexual intercourse
- Smoking
- Wart virus infection (HPV)
- Young age at first sexual intercourse
- Multiple sex partners
What causes cervical cancer?
Cervical cancer is caused by certain strains of the Human Papilloma Virus (HPV). HPV is very common in women aged 20-30 and can be sexually transmitted. The virus infects the surface cells of the genital area including the cervix, vagina and vulva and can also cause visible warts. A vaccine is now available to prevent cervical cancer.
How is it detected?
Cervical cancer, especially in the early stages, is most commonly picked up from a Pap test, but can sometimes be identified by health professionals from a woman’s symptoms. If abnormal or cancerous cells are detected from a Pap test, your doctor will refer you to a specialist (usually a gynaecologist, in particular a gynaecologist who specialises in cancer treatment).
Does an abnormal Pap test result mean cervical cancer?
An abnormal result from a Pap test (smear) means there is some change or difference in the cervical cells. Cervical cells turn over rapidly, regenerate and in this process can become abnormal or changed.
There are many reasons for a change or difference including:
- Infection
- Inflammation
- Pre-cancerous changes
The abnormal changes have been classified according to the changes seen in the surface cells (squamous cells) of the cervix. Dysplasia is the term that was previously used to define the changes in the cervical squamous cells.
Low grade changes
Non-specific changes or possible low grade squamous intraepithelial lesions are due to minor changes such as inflammation. Low grade squamous intraepithelial lesion (LSIL) includes human papilloma virus (HPV) associated changes, (mild dysplasia or CIN1).
HPV is an infection in which the virus infects the surface cells of the genital area including the cervix, vagina and vulva. It can also cause visible warts. For most women the virus will clear up by itself. In 60 per cent of women the CIN1 change will resolve spontaneously. Repeat smears are recommended to follow up these changes. HPV is very common in women aged 20-30 and can be sexually transmitted. Only certain types of HPV cause cancer.
High grade changes
High grade squamous intraepithelial (HSIL) changes includes moderate to severe dysplasia (CIN 2 + 3). These changes are precancerous and require appropriate further investigation and treatment, usually colposcopy and removal of the abnormal area on the cervix. Treatment can prevent further progress to cervical cancer.
Squamous cell carcinoma is cancer of the cervix.
For more information on Pap Tests see the Pap test article.
Treatment of abnormal Pap tests
Low grade changes
Under 30 years – Repeat Pap test in 12 months
Over 30 years – Repeat Pap test in 6 -12 months
High grade changes
Referral to a gynaecologist for colposcopy and removal of the abnormal changes. A colposcopy is an instrument like a large microscope which magnifies the cells of the cervix to visualise where the abnormality is. The cervix is painted with a solution to identify the abnormal cells. A biopsy from the abnormal area is then taken to confirm the changes. This does not require anaesthetic.
Treatment for high grade lesions
- Laser therapy
- Electrocoagulation
- Loop excision (LLETZ)
These treatments may be performed as an outpatient or as a day case in hospital. Your doctor will explain these treatments in more detail.
Treatment for cervical cancer
If diagnosed with cervical cancer you will be referred to gynaecologist who specialises in cancer treatment.
Your treatment will depend on the severity of the cancer. Treatments may include:
- Surgery to remove the cancer
- Radiotherapy
- Chemotherapy
The cervical cancer vaccine
There are two types of cervical cancer vaccines – Gardasil and Cervarix.
The Gardasil vaccine protects against HPV types 6, 11, 16 and 18.
- Types 6 and 11 are known to cause up to 90 per cent of genital warts
- Types 16 and 18 cause around 70 per cent of cervical cancer cases
The Cervarix vaccine protects against types 16 and 18.
Gardasil is approved for use in females aged from nine to 26 and males aged from nine to 15. It is recommended that girls have the vaccine around the ages nine to 12 and is best given before becoming sexually active. This is because the vaccine works best if it is received before being exposed to HPV.
Cervarix is approved for women aged 27 to 45 years, but is not covered by the Australian Government vaccination program.
How do i get the vaccine?
During 2007 and 2008 the Gardasil vaccine will be available free at school for all girls aged 12 to 18. From 2009 it will be available free to all Year 7 girls. Women aged 18 to 26 can access the vaccine free from their GP up until June 2009.
Cervarix is available from GPs and costs around $150.00 per dose. Both vaccines are administered in three separate doses over a period of six months.
Do I still need to have Pap tests if I have had the vaccine?
Yes. HPV is one of the most common STIs – four out of five women will be exposed to the virus at some point in their lifetime. Even if you have had the vaccine (either before or after becoming sexually active), it is important that you continue to have regular two-yearly Pap tests as the vaccine only protects against 70 per cent of cervical cancers.
Best Steroid Products Online
MT-2 Melanotan
|
Omnadren 250
|
Testo-C 500
|