What is a Pap test?
The Pap test is a quick and simple test used to screen women for changes to the cells of the cervix that could lead to cervical cancer.
Cells are taken with a cervical brush or spatula from the surface of the cervix (exo-cervix or ecto-cervix) and the cervical canal (endo-cervix). The cells are smeared onto a slide, fixed with a spray and sent to a laboratory where a pathologist examines them under a microscope.
Thin Prep is another type of Pap test which includes the smearing of a slide as well as putting the brush or spatula into a fluid.
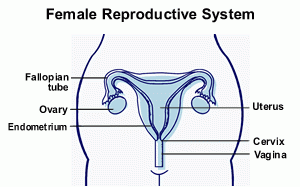 The cervix (‘neck of the womb’) is the lower part of the uterus (womb) which protrudes into the top of the vagina.
The cervix (‘neck of the womb’) is the lower part of the uterus (womb) which protrudes into the top of the vagina.
Pap tests – a screening tool
Accuracy of Pap tests
The Pap test is a screening tool. This means that the test will not diagnose 100 per cent of cervical cancers, but it is the best test available to prevent many cancers of the cervix.
There is a 10-15 per cent false negative rate for Pap tests. Similarly there is a 10 per cent false negative rate with mammograms. This means 10-15 per cent of cancers can be undiagnosed. It is important to continue regular screening.
Who should have a Pap test?
- A Pap test taken two yearly from the ages of 18-70 years will reduce each woman’s risk of developing cancer of the cervix by up to 90 per cent.
- Women should start having Pap tests about a year after their first sexual contact or between the ages 18-20, whichever is later and continue until around the age of 70 (as long as the last smear was normal).
- Lesbian women also need to have regular Pap tests.
- Women who no longer have sex should continue to have a Pap test because it may take some years for changes to develop
- Three out of four women who develop cervical cancer have never had a Pap test or had not had a Pap test in the five years before diagnosis. .
- Most women find the Pap test painless but sometimes it is uncomfortable. If the test hurts let your health professional know.
- Women over 70 who have never had a Pap test and have been/are sexually active should be screened.
When is the best time to have a Pap test?
The best time to have a Pap test is in the middle of the cycle. It is best not to have a Pap test during your period or when there is a vaginal infection such as thrush, as either blood cells or infected cells will reduce the accuracy of the reading of the test. If a test has to be repeated it is best to wait 2-3 months before repeating it so the cells can return to normal.
The Pap test samples two types of cells on the cervix – ecto-cervical and endo-cervical cells. Sometimes endo-cervical cells are not obtained and the Pap test may be repeated either in 12 months or routinely in two years. This is a common normal finding after menopause.
Thin Prep Pap test
Sometimes a Thin Prep Pap test is performed. This is a newer method for assessing cells and includes the smearing of a slide as well as putting the brush or spatula into a fluid. There is an additional cost for the Thin Prep analysis and they are non-rebatable.
This technique separates cervical cells from mucous, blood and other substances in the sample. It is used to increase the number of cells for analysis when there has previously been abnormal cells, cells unable to be accurately assessed, or when there have been too few cells to assess e.g. after menopause when the cervical cells are thin.
Frequency of Pap Tests
A Pap test should be performed every two years for the following women:
- All women aged 18-70 years who have been sexually active.
- Starting within 1-2 years of first sexual intercourse or about 18-20 years old, whichever is first.
- Lesbian women are still recommended to have two-yearly Pap tests, although it is possible other sexual activity may carry some risk there is no available data.
- Women who have ceased sexual activity should continue to have pap tests until 70 years.
- Women over 70 years may cease Pap test screening if they have had two normal smears in the previous 5 years.
- Women who are post menopausal or who are on hormone therapy should continue Pap tests until 70 years. After the menopause some women think they do not need Pap tests but because cancer may take many years to develop, it is still necessary to continue until age 70 years.
Other considerations for women:
- Women who have had an abnormal Pap test treated should have Pap tests at intervals recommended by their doctors and according to the National Health and Medical Research Council (NHMRC) guidelines. This means some women will have tests at 6 or 12 monthly intervals.
- Women who have abnormal vaginal bleeding should have a Pap test, have the bleeding investigated and then may be referred to a gynaecologist.
- Women who had a hysterectomy may need to have a vaginal vault smear (a smear taken from the top of the vagina) two yearly:
- If they have ever had an abnormal Pap test including any low or high grade lesions.
- If the hysterectomy was for cancer of the uterus or cervix.
- If the ovaries were retained after hysterectomy, these should be checked approximately 2-5 yearly.
- Have had a subtotal hysterectomy (where the cervix is left behind).
- It is important to find out if there have been any previous abnormal smears, to know the exact reason for the hysterectomy, and to have a regular check after the hysterectomy if the ovaries have been retained
Results
Normal results
A normal Pap test result means the cells are of normal appearance and the recommendation is for a repeat smear in two years.
Abnormal results
An abnormal smear means there is some change or difference in the cervical cells. Cervical cells turn over rapidly, regenerate and in this process can become abnormal or changed.
There are many reasons for a change or difference including:
- Infection
- Inflammation
- Pre-cancerous changes
The abnormal changes have been classified according to the changes seen in the surface cells (squamous cells) of the cervix. Dysplasia is the term that was previously used to define the changes in the cervical squamous cells.
Low grade changes
Non-specific changes or possible low grade squamous intraepithelial lesions are due to minor changes such as inflammation. Low grade squamous intraepithelial lesion (LSIL) includes human papilloma virus (HPV) associated changes and mild dysplasia or CIN1.
HPV is an infection in which the virus infects the surface cells of the genital area including the cervix, vagina and vulva. It can also cause visible warts. For most women the virus will clear up by itself. In 60 per cent of women the CIN1 change will resolve spontaneously. Repeat smears are recommended to follow up these changes. HPV is very common in women aged 20-30 and can be sexually transmitted. Only certain types of HPV cause cancer.
High grade changes
High grade squamous intraepithelial (HSIL) changes includes moderate to severe dysplasia (CIN 2 + 3). These changes are precancerous and require appropriate further investigation and treatment, usually colposcopy and removal of the abnormal area on the cervix. Treatment can prevent further progress to cervical cancer.
Squamous cell carcinoma is cancer of the cervix.
Treatment of abnormal Pap tests
Low grade changes
- Under 30 years – Repeat Pap test in 12 months
- Over 30 years – Repeat Pap test in 6 -12 months
High grade changes
- Referral to a gynaecologist for colposcopy and removal of the abnormal changes. A colposcopy is an instrument which magnifies the cells of the cervix to visualise where the abnormality is. The cervix is painted with a solution to identify the abnormal cells. A biopsy from the abnormal area is then taken to confirm the changes. This does not require anaesthetic.
Treatment for high grade lesions
- Laser therapy
- Electrocoagulation
- Loop excision
These treatments may be performed as an outpatient or as a day case in hospital. Your doctor will explain these treatments in more detail.
Treatment of squamous cell carcinoma (cervical cancer)
- Referral to gynaecologist who specialises in cancer treatment.
Cervical Cancer – Squamous Cell Carcinoma
Squamous cell carcinoma is the most common form of cervical cancer and can be prevented (80-85 per cent) by regular Pap tests to detect early changes. The other form of cervical cancer is adenocarcinoma accounting for 12-15 per cent. In Australia about 200 women die every year from cervical cancer and about half have never had a Pap test. Cancer of the cervix is very rare under the age of 25 years, mostly occurring in the 55-60 year age group. The progression from high grade changes to cancer takes between 1 and 30 years with an average of 10 years.
The risk factors for cancer of cervix are:
- Ever having sexual intercourse
- Smoking
- Wart virus infection (HPV)
- Young age at first sexual intercourse
- Multiple sex partners
The Cervical Cancer Vaccine
There are two types of cervical cancer vaccines – Gardasil and Cervarix.
The Gardasil vaccine protects against HPV types 6, 11, 16 and 18.
- Types 6 and 11 are known to cause up to 90 per cent of genital warts
- Types 16 and 18 cause around 70 per cent of cervical cancer cases
The Cervarix vaccine protects against types 16 and 18.
Gardasil is approved for use in females aged from nine to 26 and males aged from nine to 15. It is recommended that girls have the vaccine around the ages nine to 12 and is best given before becoming sexually active. This is because the vaccine works best if it is received before being exposed to HPV.
Cervarix is approved for women aged 27 to 45 years, but is not covered by the Australian Government vaccination program.
How do I get the vaccine?
During 2007 and 2008 the Gardasil vaccine will be available free at school for all girls aged 12 to 18. From 2009 it will be available free to all Year 7 girls. Women aged 18 to 26 can access the vaccine free from their GP up until June 2009.
Cervarix is available from GPs and costs around $150.00 per dose. Both vaccines are administered in three separate doses over a period of six months.
Do I still need to have Pap tests if I have had the vaccine?
Yes. HPV is one of the most common STIs – four out of five women will be exposed to the virus at some point in their lifetime. Even if you have had the vaccine (either before or after becoming sexually active), it is important that you continue to have regular two-yearly Pap tests as the vaccine only protects against 70 per cent of cervical cancers.
Top Steroid Products on Sale
Arimixyl
|
LIV 52
|
Clenbutaxyl
|


